A puzzling but interesting skin disorder
Around three to four weeks ago, a beautiful young lady named Jasmine consulted me online. She sent three pictures of her leg and thigh on different sites. The pictures were a “zero visibility” for making a definitive diagnosis, so I requested her to see me in person and was thankful I did, as the rashes were all over her body.
Jasmine shares her story: “Last May 7, pinkish spots appeared on my chest, upper arms and upper legs. I was thinking that it could be due to my activity of checking some condo units that had not been properly maintained for months, followed by a 10-minute walk, as the rashes appeared after I did this. The rash was not itchy or painful.
“After a few days, the spots spread out on my entire body except for my face and feet. I consulted a doctor on May 7 and was prescribed Diphenhydramine and Methylprednisolone, but there was no improvement.
“On May 10, I consulted another doctor who advised me to do some blood work. She recommended continuing the medicines I was prescribed by the first doctor but added Atopiclair cream. There was no improvement.
“On May 12, I consulted a dermatologist again for the third time, who diagnosed me with scabies. He prescribed me Permethrin cream, which I used two times for two weeks, Mometasone cream twice daily, Bilastine and Chlorpheniramine. I took these meds up to the 24th of May.
‘‘After a week of drinking these meds, some of the spots started drying up, but then the rashes did not stop from recurring.”
The skin doctor is in
And this is when she consulted me. Upon seeing her rashes, I was quite perplexed, as it really looked bizarre. It was pinkish red, some with tiny scales or scabs, but there were a lot of erosions. She said it was not itchy in general, so why the erosions (the upper roof of skin taken off), which is usually secondary to scratching?
So, I suggested she do a skin biopsy. But two days later, she called to tell me that there were new spots on her palms, a red flag for a sexually transmitted skin disease, so I did a blood test, which turned out to be positive for one and negative for the other (not conclusive).
I waited for the result of the biopsy, which turned out to be pityriasis lichenoides et varioliformis acuta, otherwise known as PLEVA or Mucha- Habermann Disease. It is named after Rudolf Habermann (1884–1941), a German dermatologist, and Viktor Mucha, an Austrian dermatologist.
Aside from the difficulty of remembering its name, which is common among eponyms in dermatology, it is also quite difficult to treat. Slow and sometimes persistent, it is a recurring dermatologic skin rash that can persist for a long time.
PLEVA is a rare disorder. The exact incidence and commonness are not known. It may occur at any age (including infants) but most frequently occurs in children and young adults.
Lympho-proliferative disorders are characterized by the overproduction of certain white blood cells called lymphocytes. These cells often accumulate in the structures and tissues of the body, potentially damaging them.
The lesions most often appear on the trunk and the arms and legs. Lesions tend to develop in small groups. A more severe variant of this disorder, known as febrile ulceronecrotic Mucha-Habermann disease, can cause life-threatening complications in adults.
The onset of PLEVA is usually sudden and marked by the development of a recurrent rash consisting of rounded, elevated lesions (papules or macules) that may be itchy and burning. These rashes are usually reddish-purple to reddish-brown and may progress to develop a blackish-brown crust (which signifies tissue death or necrosis) and bleeding (hemorrhaging).
The lesions eventually blister, often causing scarring or temporary discoloration upon healing. Luckily, Jasmine did not have this.
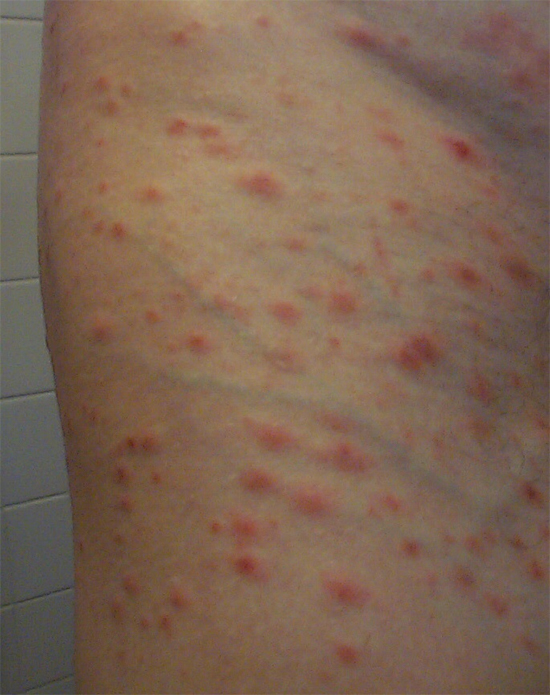
Although the trunk, arms and legs are most often affected by PLEVA, any part of the body may potentially develop skin lesions. Lesions may number only a few to more than a hundred. Lesions may resolve without treatment in a few weeks, but may recur on and off for years.
In most cases, affected individuals do not have any symptoms in addition to the skin findings. However, some individuals may have headaches, fever, joint pain (arthralgia), and a general feeling of poor health (malaise). In some cases, the swelling of nearby lymph nodes (lymphadenopathy) may also occur.
The exact cause of PLEVA is unknown. It is considered as part of the spectrum of pityriasis lichenoides, a benign group of disorders. Within this group is also pityriasis lichenoides chronica, in which the lesions are more persistent and characterized as pink-scaling round patches on the trunk and extremities. Researchers have speculated that pityriasis lichenoides occurs because of an exaggerated, inflammatory reaction (hypersensitivity) of the body to an infectious agent. However, no causative infectious agent has been identified.
Some researchers have suggested that PLEVA is a benign, self-healing lympho-proliferative disorder. Lympho-proliferative disorders are characterized by the overproduction of certain white blood cells called lymphocytes. These cells often accumulate in the structures and tissues of the body, potentially damaging them.
Treatment
PLEVA usually resolves on its own within several weeks to several months. However, in some cases various therapies to treat the condition may be used. Oral antibiotics can help to clear lesions in about 50% of affected individuals. Exposure to ultraviolet light is most helpful, particularly if the PLEVA is persistent. While individuals can show considerable improvement from summer sunlight, phototherapy (light treatments) with narrow-band ultraviolet light is an alternative for more controlled light delivery and during months that are not sunny. Methotrexate or Dapsone may be necessary in severe cases.


