Here are the things you should consider if you feel the symptoms of a COVID-19 infection
As hospital admissions have been increasing yet again in the wake of an ongoing surge of COVID-19 infections, what should one do once symptoms, which are highly similar with the common flu, manifest?
The Department of Health today, Jan. 5, reported 10,775 new COVID-19 infections, almost double the previous day, with a record high positivity rate of 31.7%. The utilization rate of isolation beds in the country is at 31%, which authorities said is still ok though the number has been steadily increasing.
Should you then rush to the hospital once you feel the symptoms of a COVID-19 infection? Here are a few of the things you should consider once you feel unwell.
First things first, what are the COVID-19 symptoms?
According to the Department of Health (DOH), the most common COVID-19 symptoms are:
- cough,
- fever,
- sore throat,
- fatigue,
- loss of taste and/or smell,
- headache,
- sore throat,
- body pain,
- rashes, and
- conjunctivitis.
The DOH noted that the symptoms are generally similar for COVID-19 infections, whether Delta or Omicron, even with regular influenza.
“It is difficult to tell by symptoms alone what caused your infection,” the DOH said in a Jan. 5 release, in reaction to circulating posts about the supposed differences in the symptoms of Delta and Omicron variants, and flu.
The agency advised that it all boils down to getting tested to confirm the type of infection or illness.
I have COVID-19 symptoms. When should I get tested?
Mind that there are two types of tests, an antigen test and a reverse transcription-polymerase chain reaction (RT-PCR) test. In an antigen or "rapid" test, an individual makes use of a pregnancy test-like kit that yields results within minutes. While the process is faster compared to RT-PCR, it’s prone to displaying false positives.
In an RT-PCR test, lab technicians study the virus’s genetic material in detail. But while it’s more accurate, the complicated process is not only more expensive but also takes more time, resulting in fewer test results in a matter of hours to even days.
The DOH said that antigen tests are best used on symptomatic patients, as they’re “fairly accurate,” but “not as reliable if used for non-symptomatic,” saying a follow-up RT-PCR may be needed to confirm the presence or absence of infection.
The DOH said it’s also best for an individual, especially one with no apparent COVID-19 symptoms, to wait until the fifth day of exposure before testing “to increase reliability of results.”
I’m symptomatic, but I’m having difficulties booking COVID-19 tests. What alternatives are available?

A makeshift hospital in Mandaluyong conducts swab test among residents. Photo by Walter Bollozos / The Philippine STAR
Edsel Salvaña of the DOH Technical Advisory Group said those who struggle to book COVID-19 tests may try to avail of home services offered by several laboratories and even local government units.
“Kung ubod ng haba ng pila, the other option is to try to get tested at home so you won’t infect anybody else,” Salvaña said during a Jan. 5 Laging Handa briefing.
Salvaña also urged Filipinos to explore telemedicine services. Here are some useful links provided by the DOH:
https://doh.gov.ph/list-of-doh-vetted-3rd-party-telemedicine-service-providers
https://doh.gov.ph/Hotline-Numbers-of-Hospitals
https://doh.gov.ph/ohcc-regional-contact-numbers
I already got tested and results came back positive. Should I rush to the hospital?
If an individual only exhibits mild symptoms, especially one who is fully vaccinated against COVID-19, the DOH said that the best thing to do is to undergo home isolation to avoid overcrowding hospitals, which need to prioritize moderate to severe cases.
“The most important thing talaga that you can do…is to stay put and not infect everybody else,” Salvaña said. “Whether you’re tested or not naman, if you’re fully vaccinated (against COVID-19), chances are it (infection) is gonna go away on its own.”
How to conduct home isolation and for how long?
The World Health Organization (WHO) said home isolation should last for 10 days from symptom onset, plus three days once symptoms cease.
In doing home isolation, the WHO advises the public to prepare a separate room or isolated place for sick family members. The area must have enough ventilation with open windows, the WHO stressed, as it poses lower risk of infection.
The organization also suggests designating a contact person (or as more commonly known in the Philippines, an authorized person outside of residence or APOR) who is not a high risk individual.
Those in the same room as the sick family member must wear a face mask. The isolated family member must also have a separate glass, plate, utensils, and bedding. Frequently touched surfaces must be cleaned and disinfected.
Symptoms must also be monitored regularly. Once danger signs like difficulty in breathing, loss of speech or mobility, confusion, and chest pain are observed, then one should call health authorities immediately.
Who should I reach out to when I test positive for COVID-19?
Try to recall where you’ve last been and who you’ve been with for the last two days or so before you got tested or started having symptoms. The Center for Disease Control Prevention (CDC) of the United States defines a close contact as someone who was less than six feet from you for 15 minutes or more.
You may reach out to your respective barangays, including the barangay emergency response team, especially if you’re living closely with your neighbors.
If it’s in a workplace setting, inform your employer immediately, more so if you are working on-site.
You must also tell your doctor, especially if you have comorbidities like diabetes or high blood pressure that puts you at higher risk.
Dr. Ashish Jha, dean of the Brown University School of Public Health, said that one must not shy away from being transparent about their positive test results.
“A lot of people think it’s some failure if you get infected,” Jha said. “A lot of people are going to get it. That is not a moral failure.”
How do I manage my COVID-19 symptoms?

Residents in Malabon line up at a small drug store to secure medicines like paracetamol. Photo by Ernie Penaredondo
The CDC recommends drinking plenty of water and getting enough rest. You may also take over-the-counter medicines like acetaminophen (or more commonly, paracetamol) to help you feel better.
In buying paracetamol, the DOH said it doesn’t necessarily have to be branded, as generic alternatives, which are also cleared by the Food and Drugs Administration, would do.
The WHO, meanwhile, advised against self-medicating, especially with antibiotics, as these only work on bacterial infections.
“COVID-19 is caused by a virus, so antibiotics do not work. Antibiotics should not be used as a means of prevention or treatment of COVID-19,” the WHO said.
Health authorities also said one could avoid getting sick through a healthy lifestyle of eating fruits and vegetables, limiting intake of fatty and high cholesterol food, doing exercises regularly, as well as taking Vitamin C, Zinc, and herbal remedies like turmeric and ginger.
What are the other ways to deal with COVID-19?
The CDC said those who are sick should wear masks that cover the nose, mouth, and chin. They must have clean hands before wearing and removing the masks, and after touching it any time.
Several health authorities, meanwhile, have long been recommending using N95, KN95, or KF94 masks due to their layers of protection. Surgical masks should also be three-ply. As for those with cloth masks, they must consider putting surgical masks underneath through proper layering.
The DOH has also recommended double masking and pairing masks with face shields.

Shoppers roam Ilaya Divisoria last Jan. 3. Photo by Michael Varcas / The Philippine STAR
The public must also clean their hands frequently with alcohol-based hand rub or soap and water, the CDC said. They must cover their mouths and noses with a bent elbow or tissue when coughing or sneezing, and used tissues must be disposed of immediately.
Surfaces that are regularly touched like door handles, faucets, and phone screens must be cleaned and disinfected frequently.
As much as possible, the CDC said the public must avoid the 3Cs: spaces that are Closed, Crowded, or involve Close Contact.
If meeting with peers outside can’t be helped, it must be in outdoor settings with enough natural ventilation. Indoor settings must have open windows as much as possible.
Ultimately, the best way to deal with the pandemic is to get vaccinated against COVID-19 as soon as possible. For those who have already received their full doses for the two-dose series, you must get your booster shots once eligible. Visit the Facebook pages and websites of your respective LGUs to know the next earliest vaccination schedule available.
I’ve already recovered from COVID-19 in the past. Should I be less worried about getting reinfection?
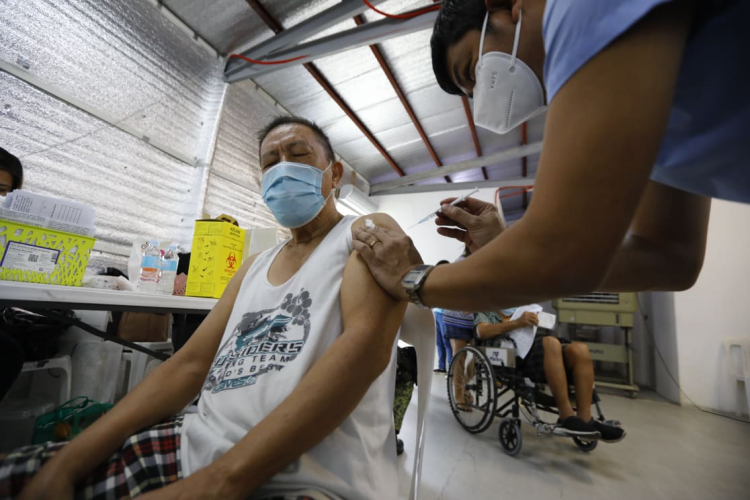
A Marikina resident takes his COVID-19 booster shot at the Marikina Sports Complex mega vaccination site. Photo by Walter Bollozos
Apparently, those who have contracted the disease are still at risk of testing positive all over again, as the degree of protection from a previous infection varies from person to person.
But those who have been vaccinated against COVID-19, especially those who have received their booster shots, have a stronger line of defense against the disease.
A CDC study last August 2021 suggested that unvaccinated individuals are more than twice as likely to be reinfected with COVID-19.
"What we want to emphasize is to get the unvaccinated vaccinated," acting presidential spokesman Karlo Nograles said in a Jan. 5 Laging Handa briefing. "Iyong mga mild cases na nakikita natin ay from the vaccinated. We cannot say the same thing about the unvaccinated."


