The importance of narrative medicine
Every patient has a story that goes beyond the symptoms they bring into the doctor’s office. Those stories can elucidate how a person got sick, the crucial stage or turning point that made them seek help, and perhaps, most importantly, the challenges they faced in trying to get better.
Stories can offer the kind of contextual richness that promotes and nourishes empathy, prompting a medical provider to switch from asking, “How can I treat this disease?” to “How can I help my patient?” The difference may seem subtle at first, but knowing how to get patients to share their stories can be transformative in improving patient care, as proponents of this approach called narrative medicine are saying.
In a nutshell, narrative medicine draws on the study of art and literature to enhance the listening and observation skills of medical or health providers in general and to expand their view of patients, to encompass more than just the routine medical histories and physical examinations that they do.
“Narrative medicine is a commitment to understanding patients’ lives, teaching and caring for the caregivers, and giving voice to the suffering.”
One of the core principles of narrative medicine is that receiving patients’ stories helps to build empathy in medical professionals, which, in turn, improves the quality of care and benefits patients by boosting their recovery faster.
Indeed, recent studies have shown that higher levels of healthcare provider’s compassion may be associated with more positive outcomes in patients’ quicker recuperation.
Case #1: A 72-year-old patient who arrived from the US went to a derm clinic for a checkup. Upon consultation, she was offered several procedures on the same day. I think five procedures were done all at the same time. After two days, she developed a small blister on the forehead, which spread so fast that her entire right face was covered with a yellow crust with blisters that were surrounded by a large, purplish-red patch. Her eyes were swollen and exuded a pus-like material that made it difficult to open her eyes. She consulted with a dermatologist, who diagnosed her with a severe form of allergy and gave her medicines for this. Unfortunately, there was not much improvement, so she visited me. Upon seeing her, I thought at first that I was dealing with a bacterial infection alone but after examining her thoroughly, I concluded that not only did she have a bacterial infection but a viral infection as well. So I gave her an antibacterial and antiviral treatment and taught her how to boost her immune system so she could fight both types of infections faster and prevent severe scarring, plus damage to other organs of the body, especially the eyes. In the eyes, glaucoma, cataracts, chronic or recurrent uveitis, corneal inflammation, scarring and neovascularization, numbness and vision loss is possible.
In severely compromised patients like those with cancer, HIV, or those under immunosuppressive treatment, visceral involvement with pneumonitis, encephalitis, hepatitis, and retinal necrosis can occur. And, in the case of a bacterial infection like this, cellulitis, septicemia, zoster gangrenosum, necrotizing fasciitis, which are life threatening, may also occur.
Case # 2: A 16-year-old patient came to my clinic because of nodular acne on her chest and back, associated with scars. The patient presented with good general health conditions, with neither personal nor family history of severe acne, endocrine, or rheumatologic disorders. Patient also denied intake of medications that might cause acne vulgaris or acneiform eruptions, like steroids, lithium, phenytoin, isoniazid, and B-complex vitamins. Because of the severity, systemic anti-acne antibiotic therapy (lymecycline 300 mg daily for eight weeks) was prescribed.
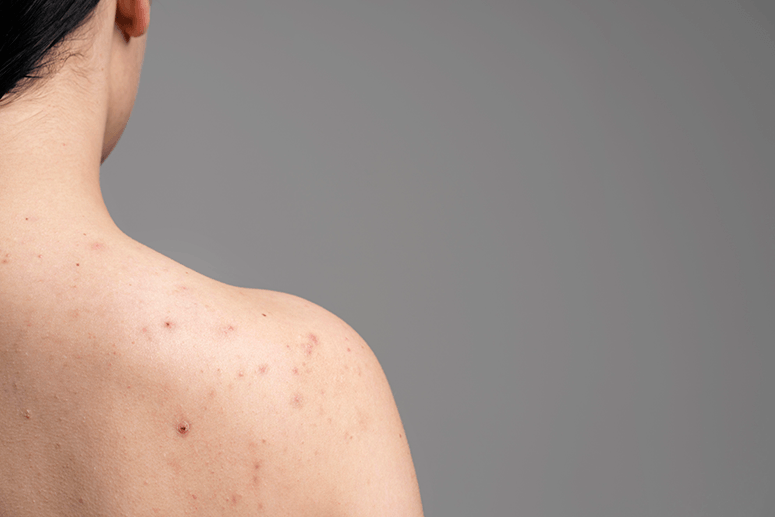
After five days of treatment with this drug, a dramatic onset of multiple painful, ulcerated nodules on the trunk, associated with mild fever, headache, and joint stiffness occurred. Blood tests revealed a white blood count of 12,340/mm2 and an erythrocyte sedimentation rate of 45 mm/h, without any other abnormality. Despite joint pain, referral to a rheumatologist showed an absence of functional impairment, and ultrasonographic imaging of the right knee and the left shoulder revealed no significant alterations.
Based on clinical and laboratory findings, diagnosis of acne fulminans (AF) was made. Lymecycline was withdrawn, and corticosteroid therapy was prescribed. Twenty-one days later, significant improvement was noted. While tapering down corticosteroid dosage, isotretinoin was introduced and prednisone was gradually reduced at the same time. Five months later, the inflammatory lesions of acne had almost completely resolved into scars.
Indeed, recent studies have shown that higher levels of healthcare provider’s compassion may be associated with more positive outcomes in patients’ quicker recuperation.
Case # 3: A 65-year-old woman was referred to me by the friend of a relative due to a non-healing large ulcer at the ankle. First it was her right leg. The ulcerations finally healed after a very, very long time, leaving a very large, white depressed scar. It was a really unsightly scar surrounded by a brownish discoloration at the periphery. After several months, a small ulceration started to develop on her left leg and at the time of presentation at my clinic, it was already quite deep and the size of half of my palm or even larger. This time it was scarier to look at. Upon physical examination, I noticed the large, bulging varicose veins on her left leg, including the thigh area. There were actually no more areas without the bluish large vein in sight. The right leg, on the other hand, also presented with many large, reticular veins (these are the visible veins below your skin that appear blue-purple in color, but don’t bulge as varicose veins do) all over the legs and thigh areas, too.
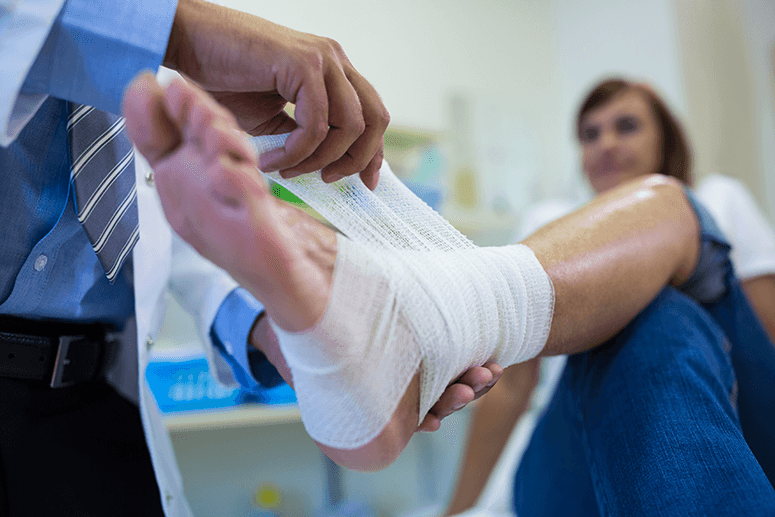
Aside from these, I noted an inverted “Coca-Cola bottle” sign, where the legs are of normal size but the lowest third of the leg is thinned out due to the thickening and tightening of the skin. I started treatment right away, and after the first session, the ulceration was 30-percent smaller and shallower. Bulging of the veins disappeared and the other reticular veins were also less visible. Hard lumps, however, could be seen and felt. These lumps will disappear gradually with time. The patient felt better: less tired, less heaviness over the leg areas; she felt optimistic and relieved that her suffering would be over soon.
I am happy for all these patients and thankful for their recovery.


